This page is for my current patients only
此網頁只供我現時病人閱讀

Background 背景
When the intervertebral disc prolapsed or the ligament behind the vertebrae thickened or turned into bone, the tunnel for the spinal cord and nerve root traveling through would be occupied. As a result, the pinched spinal cord or nerve root space would cause neuropathic pain, weakness, numbness, clumsiness over the hands and legs. Patients might have fallen easily and repeatedly. He or she might have difficult in using chopstick and buttoning. Severe cases might note urine leakage upon coughing, straining after passing water revealed residual urine, and drop of stool when farting.
The surgery aims at removing the prolapsed disc and part of the thickened ligament (called posterior longitudinal ligament, PLL). It will decompress the pinched spinal cord and nerve root and provide the best environment for them to recover. Least, the neurological deficit would not deteriorate.
In order to create enough space for nerve root, removing part of the bone spur of the small joint (Joint of Luschka) might be performed concurrently (called foraminoplasty).
After the decompression, the space would have 3 different ways to get restored,
- Artificial Disc Replacement (ADR)
Using minimal invasive technique, a small wound of 45mm is made on the right side of the throat along the skin crease. It can preserve near normal neck motion and avoid stress on adjacent levels, which are usually degenerative in some extend.
- Cervical Spinal Fusion (Anterior Cervical Discectomy and Fusion, ACDF)
Gold standard for restoring neck stability and alleviating neck pain. However, after fixing the segment, stress will be heighten on adjacent levels and might accelerate degeneration.
- Combination (Hybrid procedure)
When the number of affected levels is more than 2, the third level cannot be implanted with an artificial disc according to protocol. Using a combination of both artificial disc and fusion is called hybrid construct.
To enhance safety margin, the following technologies would be used in general
- Microscope
It allows the operation under magnification, thus decreasing the error
- Intraoperative neuromonitoring
By passing electrical signal through the operating segment, we can monitor the neurological function and save some catastrophic case. The result also can indicate the success of decompression on table.
當椎間盤凸出或椎體後的韌帶增厚或骨化時,原本安放脊髓和神經根的通道會被佔據。結果,脊髓或神經根會受擠壓,因而引起手、肩、上背甚或腿上的神經痛,乏力,麻痺,遴迍(音「論盡」)。患者可能容易反复跌倒。在使用筷子和扣釦時可能會有困難。嚴重者大小便控制有問題,例如咳嗽有滲尿,小便後再谷會發現遺尿,放屁時可能掉出糞便。
手術旨在去除凸出的椎間盤和部分增厚的韌帶(稱為後縱韌帶,PLL)。它將為受壓的脊髓和神經根減壓,並為它們提供最佳的康復環境。即使壓壞的神經不能恢復,至少,神經功能受損情況不會惡化。
為了為神經根製造充足空間,可能同時切除小關節的骨刺(Luschka關節)的一部分(稱為神經管道成形術)。
減壓後,原本的椎間盤空間有3種不同的方式重塑,
- 人工椎間盤置換(ADR)
使用微創技術,在喉嚨的右側沿著皮膚的摺痕打開一個45mm的小傷口。手術後頸部運動範圍大致正常,並能夠避免在相鄰的椎間盤產生過量的負荷,理論上可避免加劇退化。
- 頸椎融合術(前路頸椎間盤切除和融合術,ACDF)
它是恢復頸部穩定性和減輕頸部疼痛的黃金標準手術。但是,在固定該節段後,相鄰的椎間盤需抵受更大的負荷,並可能加速退化。
- 組合(混合程序)
當受影響範圍多達3節椎間盤,根據建議,不能連續植入三節人工椎間盤。所以需結合使用人工椎間盤和融合術,此稱為混合構建。
為了提高安全度,一般會附以以下技術
- 顯微鏡
它允許放大的立體目視操作,從而減少誤差
- 術中神經監測
利用電信號通過手術的脊髓段落,我們可以得知神經功能,從而避免一些災難性情況的發生。檢測結果還可以標示減壓效果
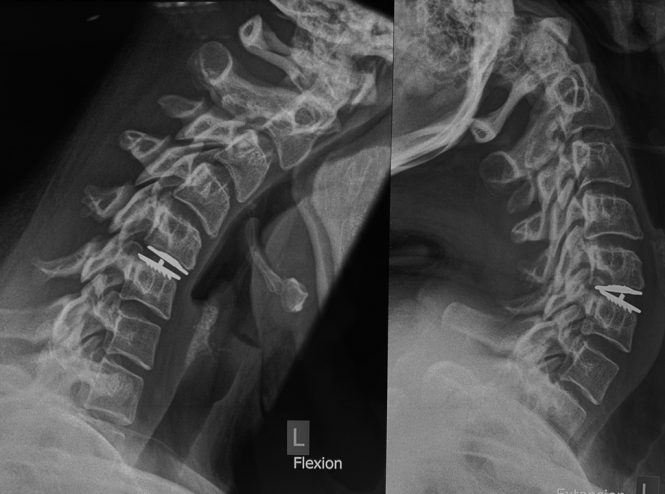
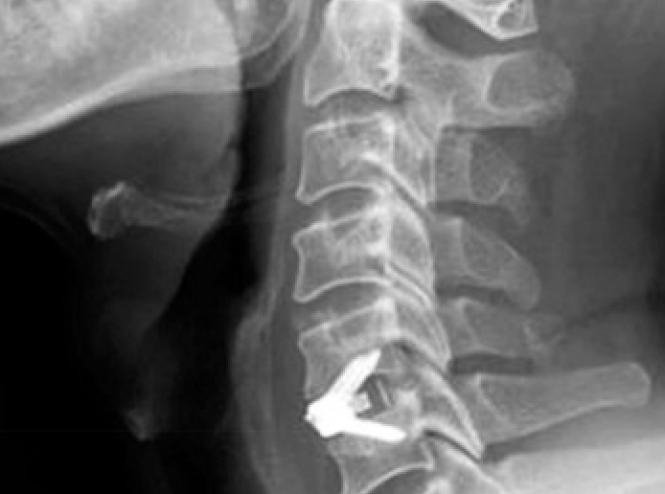
Indication 適應症
- Cervical Radiculopathy 頸神經根病變
- Cervical myelopathy 頸脊髓病變
- Neuropathic pain due to prolapsed disc 因椎間盤引起的神經痛
- Cervical Spinal Stenosis 頸椎管狹窄
- Discogenic neck Pain 椎間盤源性頸痛
Preparation 預備
- Pre-op workup 手術前身體檢查
- Walking >10000 steps a day 堅持每天1萬步強化背及腿肌
- Do more deep breath 多深呼吸
- Continue usual medication on operative day 手術當天照常食藥
- No food or drink for 6 hours 手術前6小時禁食及禁喝水
- Admit to hospital 3 hours before surgery 手術前3小時到醫院
- Inform your relative despite surgery takes 3 hours, you will return no earlier than 4 hours. 通知家人即使手術需3小時,但回病房可能是4小時後
Risk 風險
While all medical and nursing professionals endeavor to provide best and safest practice, complications still would occur.
General operative risks including heart attack, stroke, wound infection, wound hemorrhage, urinary tract infection, deep vein thrombosis, scar pain and keloid etc, is possibly encountered.
Hoarseness is not uncommon but usually resolves in days and seldom has consequence. Permanent hoarseness due to vocal cord palsy carries risk lower than 1%.
Dry eye, contracted pupil, drooping eyelid might occur in 0.1% cases.
Single nerve root injury is rarely occurred risk, with risk less than 1%.
Other rare complications include major neurological deficit, esophagus leakage (0.03%), vascular injury have been reported. Risk is higher for older patients, more significant compression on the spinal cord, and more prolonged compression period. Anatomical variants also carry more risk.
Same or adjacent level recurrence is around 10%, which should be counted as natural course rather than complication.
儘管醫生和護士都會盡最大努力提供最佳和最安全的治療,但併發症仍會發生。
一般手術可能會遇到的風險,包括心臟病發作,中風,傷口感染,傷口出血,尿道感染,深層靜脈血栓形成,傷口疼痛及增生等,這手術也不例外。
聲沙雖並不罕見,但一般會於數日消退而不留後遺症。 持續聲沙,因為聲帶神經受損,出現率少於1%。
瞳孔收縮,眼乾,眼皮半墮發生機率為0.1%。
單根神經根損傷是很少遇上的風險,發生率少於1%。其他罕見的併發症包括嚴重的神經功能缺損,食道損傷(0.03%),血管受損等。
老年患者的風險更高。脊髓受壓更嚴重或受壓時間較長的患者,或先天結構異常也會有更高的風險。
同位或近位復發大概為10%,但這屬疾病的自然進程,不屬併發症。
Budget Estimation 預算費用
CPT code and RVU is as follows
- 22551 Arthrodesis, anterior interbody, including disc space preparation, discectomy, osteophytectomy and decompression of spinal cord and/or nerve roots; cervical below C2, RVU 25.00
- 20930 Allograft, morselized, or placement of osteopromotive material, for spine surgery only (list separately in addition to code for primary procedure).
- 22845 Anterior instrumentation; 2 to 3 vertebral segments (list separately in addition to code for primary procedure). RVU 11.94
- 22853 Insertion of interbody biomechanical device(s) (e.g., synthetic cage, mesh) with integral anterior instrumentation for device anchoring (e.g., screws, flanges) when performed to intervertebral disc space in conjunction with interbody arthrodesis, each interspace, RVU 4.25
- 22856 Total disc arthroplasty (artificial disc) anterior approach, including discectomy to prepare interspace (other than for decompression) single interspace: cervical. RVU 24.05
CPT碼和RVU如下
- 22551關節固定術,前椎間融合器,包括椎間盤間隙準備,椎間盤切除術,骨贅切除術和脊髓和/或神經根減壓; 頸椎低於C2,RVU 25.00
- 20930同種異體移植物,鋸齒狀或骨刺激性材料的放置,僅用於脊柱手術(除了主要程序的代碼外,單獨列出)。
- 22845前方器械; 2至3個椎骨節段(除了用於主要手術的代碼外,單獨列出)。 RVU 11.94
- 22853插入椎間盤生物力學裝置(例如合成籠,網孔)並結合整體前部器械進行器械錨固(例如螺釘,扣片),結合椎間盤關節固定術對椎間盤間隙進行固定,每個間隙,RVU 4.25
- 22856全椎間盤置換術(人工椎間盤)前入路,包括椎間盤切除術以準備間隙(除減壓以外)單個間隙:頸。 RVU 24.05
Estimation based on general ward as in Aug-2020,
- Surgeon fee $96,000 (Single level TDR); $144,320 (Single level ACDF with bone graft)
- Anaesthetist fee $32,000 (Single level TDR); $48,106 (Single level ACDF with bone graft)
- Ward round $1,200/day
- Hospital charge $160,000 (Single level TDR); $150,000 (Single level ACDF with bone graft)
Total $288,000 (Single level TDR); $342,426 (Single level ACDF with bone graft) around
根據普通房於2020年8月進行的估算,
- 外科醫生費$96,000 (單節人工頸椎間盤替換術); $144,320 (單節前路頸椎間盤切除和融合術)
- 麻醉師費$32,000 (單節人工頸椎間盤替換術); $48,106 (單節前路頸椎間盤切除和融合術)
- 巡房費$1,200
- 醫院費$160,000 (單節人工頸椎間盤替換術); $150,000 (單節前路頸椎間盤切除和融合術)
總計$ 288,000 (單節人工頸椎間盤替換術); $342,426 (單節前路頸椎間盤切除和融合術) 左右
Reference figures from private hospitals 醫院提供的參考數據
St Paul’s Hospital 聖保祿醫院
Median Charge 收費中位數 (Single level ACDF with bone graft 單節前路頸椎間盤切除和融合術)
- Doctors’ fee 醫生費 $160,800
- Hospital charge 醫院收費 $107,800
- Total 總費 $268,600
Cannosa Hospital 嘉諾撒醫院
Median Charge 收費中位數 (Single level ACDF with bone graft 單節前路頸椎間盤切除和融合術)
- Doctors’ fee 醫生費 $121,500
- Hospital charge 醫院收費 $122,494
- Total 總費 $243,994
Baptist Hospital 浸會醫院
Median Charge 收費中位數 (Single level ACDF with bone graft 單節前路頸椎間盤切除和融合術)
- Doctors’ fee 醫生費 $125,400
- Hospital charge 醫院收費 $123,402
- Total 總費 $248,802
Adventist Hospital 港安醫院
Median Charge 收費中位數 (Single level ACDF with bone graft 單節前路頸椎間盤切除和融合術)
- Doctors’ fee 醫生費 $135,333
- Hospital charge 醫院收費 $205,381
- Total 總費 $340,714
Post-op care 術後照顧
- Control inflammation with regular usage of anti-inflammatory drug.
- The wound is covered by a waterproof dressing. You can shower, but do not take bath or rub on it. Keep the dressing intact, there is no need to change it regularly.
- You can sleep on your back or your side, without or with a thin pillow. But when you lie in bed, please make it an inclined bed or simply sleep on sofa. Keeping the neck vertically above the chest is important for swelling to subside.
- Walking and standing are encouraged.
- Pay attention to ergonomics especially when working on phone.
- If need, drinking cool water might help.
- Tuck the tongue out every now and then to mobilise the throat.
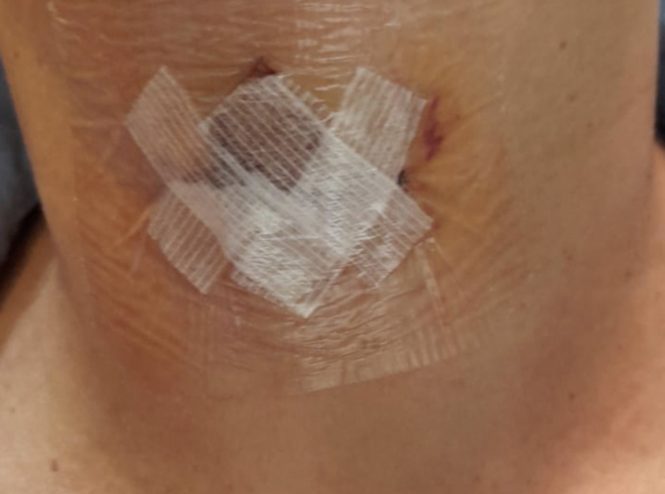
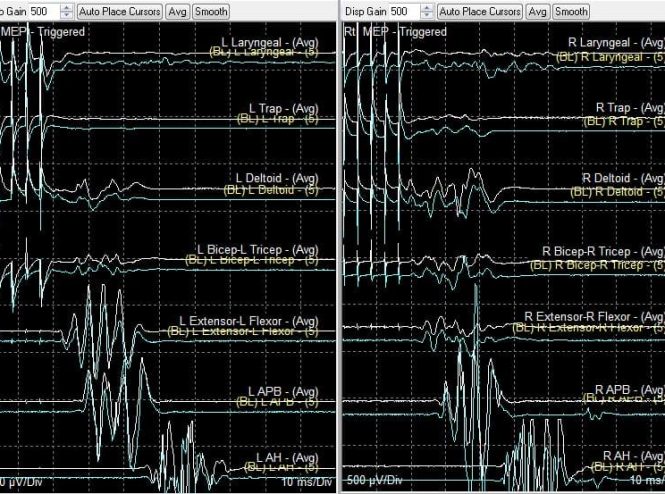
- 定時服藥,控制發炎
- 傷口已用防水敷料覆蓋。所以您可以淋浴,但不要浸澡或捽這敷料。你只需保持敷料完整,無需定期更換它。
- 您可以仰臥或側睡。如要使用枕頭,選擇薄一點的。首數天用斜床或可挨低的沙發,令頸部垂直位置高於胸口,以利消腫。
- 多步行和站立
- 日常注意活動姿勢,尤其避免低頭看手機。
- 如有需要,可多喝凍水。
- 多做開口伸脷動作,活動咽喉,避免黏連。
Early Post-op Complication 手術後早期併發症
Notify surgeon in case you have
- Persistent fever of more than 37.5 Celcius
- Chills and rigor
- Wound pain despite rest
- Wound redness and swelling
- Purulent discharge from wound
- Calf pain
- Ankle swelling, progressive
- Sudden onset of shortness of breath
- Chest pain
如發現以下情況,要立即通知醫生
- 持續高燒(口探高於攝氏37.5度)
- 發冷打顫
- 無論運動或休息時,傷口痛楚都持續增加
- 傷口持續發紅腫脹
- 傷口有膿液
- 小腿愈見痛楚
- 小腿、腳踝和腿部腫脹持續增加
- 突發性的氣促
- 胸口突然疼痛
Rehabilitation after Day 14 手術後2週復健
Range of Motion Exercise:
- Rotation, Flexion-Extension, Lateral-Flexion:
Turn left and right, within comfort zone only, hold at end of range for 5 seconds, repeat 10 times for each side.
Repeat for Flexion and Extension (F/E ROM), and Lateral bending (lateral flexion), also within comfort zone. Do not stretch it for additional range.
Postural Adjustment:
- Retraction exercise
Stand against the wall, with shoulders, buttock and heels in contact with the wall. Try to retract the neck so that your occiput (back of your head, not the top of your head) reaches the wall. Hold for 10 seconds, then relax. Rest for 10 seconds. Repeat the whole set of exercises 10 times. - Regain cervical lordosis
Lie on your back, roll a small towel behind the neck. Lie on it but maintain the back of your head is in touch of the floor, stay for 1 minute. Roll the towel bigger till it still allow your head on floor. For the biggest towel roll, lie on it for 5 minutes. Stand up and walk around, 10 minutes later, repeat the process. Do 6 times a day.
Caution on neck care:
- Do not stretch, twist, or bend your neck suddenly to avoid spraining your neck.
- Avoid bending the neck for more than 5 minutes. If need to work on phone, lift it up to eye level.
- You can sit in the office for a long hours in 2 weeks after the operation, and do manual lifting no earlier than 3 to 4 months.
- Increase the amount of activity gradually and avoid strenuous exercise, especially running and jumping.
- Sex life can start at 6 weeks after surgery.
- Avoid excessive neck fatigue within one year.
活動範圍運動:
- 左右轉動,屈伸,側彎
在舒適區域內向左旋轉,在範圍末端保持5秒鐘之後回中,再轉右到範圍末端保持5秒鐘,之後回中,每側重複10次。
同樣在舒適區域內重複進行低頭屈伸運動(下巴觸胸)和側彎(耳觸肩)。不要勉強伸展。
姿勢調整:
- 收頸運動
靠牆站,令雙肩,臀部和腳跟都觸到牆壁。嘗試縮回頸部,以使後枕(頭後部,而不是頭頂)觸及牆壁。保持10秒鐘,然後放鬆。休息10秒鐘。重複整套練習10次。 - 恢復頸椎前弓
卧躺,在脖子後面卷一條小毛巾。躺在上面,但要保持後枕能夠觸地,保持1分鐘。將毛巾卷大些,直到它仍然可以讓你的後枕觸地。用這卷最大的毛巾墊頸,躺5分鐘。站起來走走,十分鐘後,重複此過程。每天做6次。
注意頸部護理:
- 不可突然伸張、扭轉、彎曲頸部,以免扭傷頸部。
- 避免低頭曲頸超過5分鐘。如果需要用手機,請將其抬起至視線水平。
- 手術後2週可長時間坐辦公室工作,3到4個月後才可做體力勞動工作。
- 漸進式增加活動量,避免劇烈運動,尤其是跑步跳躍。
- 性生活手術後6周可恢復。
- 一年內避免頸部過度疲累。
Reference 參考文獻
- Wang JC, Buser Z, Fish DE, et al. Intraoperative Death During Cervical Spinal Surgery: A Retrospective Multicenter Study. Global Spine J. 2017;7(1S):127S-131S. https://pubmed.ncbi.nlm.nih.gov/28451484/
- Micheal J Lee, Mark A Konodi, Amy M Cizik, et al. Risk Factors for Medical Complication after Cervical Spine Surgery: a multivariate analysis of 582 patients. Spine (phila Pa 1976) 2013 Feb 1:38(3):223-228 https://pubmed.ncbi.nlm.nih.gov/22805344/
- Mullins J et al. Retrospective single-surgeon study of 1123 consecutive cases of anterior cervical discectomy and fusion: a comparison of clinical outcome parameters, complication rates, and costs between outpatient and inpatient surgery groups, with a literature review. J Neurosurg Spine. 2018 Jun;28(6):630-64 https://pubmed.ncbi.nlm.nih.gov/29600910/
- Patel Np et al. Esophageal injury associated with anterior cervical spine surgery. Surg Neurol. 2008 Jan;69(1):20-4

